Table of contents
- David Weintraub, owner of Bodyworks DW writes about working with clients experiencing PTSD symptoms and how advanced massage for stress can make a fantastic addition to other therapies!
- How I got started with massage for PTSD & chronic stress
- Practicing massage for stress and PTSD has profoundly changed how I work with ALL clients. Most of whom are also dealing with stress symptoms they aren’t even aware of.
- First of all, what exactly is stress? When does it become chronic stress?
- Our survival systems are supposed to be turned off once you are safe and fed. So that you pass out and heal until tomorrow.
- Sympathetic Nervous System = Freeze, flight, fight (or Hide, Run, Fight)
- Parasympathetic Nervous System = Rest & Digest
- What might occur if you can’t turn off the sympathetic and re-engage the parasympathetic?
- Here are some possible symptoms of chronic stress:
- What is PTSD?
- Here are some of the potential symptoms that PTSD can cause:
- How can massage for stress and PTSD help….if it’s my brain?
- Improving Breathing: where massage for stress can really help
- Massage for Stress and PTSD can help reset normal breathing and allow rest and relaxation again
- We hear about all sorts of “correct” ways to breath:
- Guess what actually happens when you try to control your breath?
- However, if you tend towards even, sustained control and constant drive, you probably need to practice far less breath control.
- And once the first injury happens, they start piling onto each other. Quickly.
- So it’s not unusual for a client to have a short cry for no logical reason on the table.
- If you are dealing with symptoms from chronic stress and/or PTSD, we’d love to help with massage for stress and PTSD!
- Citations
- Further Reading
- https://bodyworksdw.com/blogpost/advanced-massage-for-stress-ptsd-part-1-what-is-chronic-stress-what-is-ptsd/#h-here-s-a-good-stress-relief-exercise-to-help-you-in-the-meantime-yes-it-says-for-back-aches-but-it-s-a-good-all-around-stress-relieverHere’s a good stress relief exercise to help you in the meantime. Yes it says for back aches but it’s a good all around stress reliever!
How I got started with massage for PTSD & chronic stress
When I started massage school, I didn’t envision myself working on clients in need of massage for stress and PTSD. My hero was and is Ida Rolf (1), who created the concept of structural integration. My focus was postural realignment and injury recovery. Throughout my career, I’ve used Ida’s work as a guide, and slowly but surely made my own sequences and style.
However, along the way, many PTSD clients have found me and asked if I could help them. I’ve never been shy about trying new things as a massage therapist. I told them I’d be happy to try. So I started an in-depth study of the body’s survival systems. And how massage for stress and PTSD can help adjust them to a healthier balance. I’ve now worked with hundreds of survivors dealing with PTSD symptoms from many different kinds of trauma. And along the way, developed specific massage techniques that have definitively helped lower and dissipate symptoms from stress and PTSD.
Practicing massage for stress and PTSD has profoundly changed how I work with ALL clients. Most of whom are also dealing with stress symptoms they aren’t even aware of.
It’s been a decade since my first diagnosed severe PTSD client walked into my studio. They had very noticable and overwhelming symptoms that were overt and impacted them daily. Working with them and seeing their symptoms has helped me see the far more subtle stress symptoms that the rest of us generally exhibit. I now view stress and PTSD symptoms are far more common than we have previously thought. Incorporating stress reduction work into sessions with all my clients has vastly improved their recovery time. Especially from the pain injuries they came in for.
I now view PTSD and chronic stress as a spectrum that exists between healthy and balanced, and overburdened and unbalanced. Which most of us are on at some point in our lives. Most of us exist on the low end of the spectrum and wouldn’t qualify for a clinical diagnosis for PTSD from a mental health professional. However, it can still be valuable to explore the idea that you’ve got a bit of it. And that you could use some help and some tools for toning it down. Massage for stress and PTSD can certainly provide those!
First of all, what exactly is stress? When does it become chronic stress?
Clinically, stress is simply the way that your brain and body reacts to the demands put upon it (2). It occurs any time we challenge our system to try something slightly outside of our comfort zone. It includes a set of physiological responses to allow your body to meet the increased demands. These include hormonal changes such as increased adrenaline and cortisol. These hormones induce increased heart and breathing rates as well as masking pain. Your body pulls blood from the digestive organs and brain. And pumps it into skeletal muscles to allow you to hide, run, or fight.
These systems evolved to deal with immediate physical dangers and challenges. Dangers that included being attacked by a predator, stalking prey, or being injured. These survival systems were meant to be engaged to help you survive a dangerous event.
Our survival systems are supposed to be turned off once you are safe and fed. So that you pass out and heal until tomorrow.
Unfortunately, our body interprets the imagination of danger to be equal to the real thing. So we are engaging these systems all the time for things that aren’t immediately dangerous. Like finishing a report that is due on Monday. Or a traffic jam (3). Many of us get stuck in stress mode due to constant stressful triggers that we unconsciously interpret as danger. Even when we are physically safe.
This “always on” type of stress is what we call chronic stress.
Sympathetic Nervous System = Freeze, flight, fight (or Hide, Run, Fight)
Parasympathetic Nervous System = Rest & Digest
In and of itself, stress is neither a good nor a bad thing. But it’s meant to be a “use sparingly” kind of system, and it is absolutely meant to be turned off. Anatomically, you have two sets of nervous systems acting behind the scenes, your sympathetic and your parasympathetic. Remember those as we’ll be referring to them a lot!
Notice the second system, the parasympathetic nervous system and what it’s in charge of. It’s supposed to turn on when the danger passes and you are back home safely in your cave with food. It’s the time your body needs to recover from stress, heal, digest, and reset for the next stress event.
What might occur if you can’t turn off the sympathetic and re-engage the parasympathetic?
Have you been sleeping less than a full 8-9 hours a night? Waking up without feeling refreshed? Having digestive issues such as IBS, ulcers, colitis, loss of appetite or stress eating?
Here are some possible symptoms of chronic stress:
- Insomnia and or other sleep issues
- Digestive issues
- Wear and tear injuries, especially ones happening with noticeably greater frequency
- Emotional outbursts or a lack of access to emotions
- Headaches and TMJ
We normally equate “stress” with a mental feeling of “not being able to hold it together.” However, in order to achieve “holding it together” we often subject our bodies to chronic physiological stress. A pattern that has long term detrimental effects on our health. Our systems are not designed to run “evenly” all the time, especially not at high output. We need to be able to turn the engine off, let it cool down, change the proverbial oil, etc. Otherwise things start to break down over time.
What is PTSD?
PTSD stands for post traumatic stress disorder (4). PTSD is caused by a variety of traumatic events either experienced or witnessed by a person. Experienced events include but are not limited to various forms of abuse, rape, and personal injury. Witnessed events can range from losing a loved one, natural disasters, serious accidents, war, terrorism, and more. Many events include both an experienced form and a witnessed form of trauma.
PTSD and chronic stress can have many similarities. However, with chronic stress, the person is generally stuck in sympathetic mode.
With PTSD a person can swing wildly between the two modes.
How PTSD is different from chronic stress
Physiologically, we can define PTSD as an out of control threshold between our sympathetic and parasympathetic nervous systems. In some cases, it shows up as a very low threshold that triggers a massive stress response at the slightest bit of upset. Put differently, severe trauma creates a state where relaxation is no longer trustworthy. A PTSD sufferer must stay in the heightened alert state of stress in order to feel safe. Dropping out of the sympathetic nervous system into rest or relaxation will trigger an uncontrolled and often severe episode of stress.
Conversely, PTSD can also show up in cases where the trigger for stress to be “set” much too high. This can cause chronic depression, catatonia, fainting, and other types of avoidance mechanisms. In these cases, severe trauma creates a state where any stress is terrifying, and therefore avoided. It’s like our body can’t adjust to a stressful situation and doesn’t switch on to handle it.
As the word “post” implies, PTSD can trigger symptoms in sufferers long after the actual event occurs.
PTSD is often depicted in the context of soldiers returning from war. With symptoms such as intrusive thoughts and flashback memories. While these are definitely common symptoms they are not the only ones possible.
Depending on the symptoms, PTSD can be immediately dangerous. Such as cases where the sufferer has a break with reality or a violent outbreak. It can also have more subtle and longer term detrimental health effects. Systems break down faster without adequate rest and healing time under chronic stress triggering.
Here are some of the potential symptoms that PTSD can cause:
- Intrusions: such as unwanted memories, distressing dreams, and flashbacks. In extreme cases these can take over normal reality causing the sufferer to relive the experience. Or feel like they are having it for the first time despite what is actually happening around them.
- Avoidance: behaviors such as withdrawal and depression, often as part of a subconscious effort to avoid remembering the event(s).
Changes in Mood or Cognition: This can include lost or masked memories, distorted and negative thoughts and feelings, wrongly remembered causes for the event(s), and other alterations - Changes in Coping and Emotional Balancing: which may result in hair trigger bouts of anger or sadness, self-destructiveness, loss of sleep or ability to focus
If you are experiencing any of the above on a regular basis, it’s worth talking to a mental health professional. Especially if you have had a known traumatic event or events that could cause PTSD. They may or may not give you a clinical diagnosis for PTSD. Regardless, they can likely help you sort through your thoughts and feelings. And learn better coping mechanisms that will help you curb any symptoms that are preventing you from fully enjoying life on a daily basis.
How can massage for stress and PTSD help….if it’s my brain?
Well the first thing to realize is that it ISN’T just all in your brain. And that your brain and body functions are not nearly as separated as we might think. We hear all the time about the “mind/body” connection. But generally in some sort of vague hocus pocus kind of way. That makes it sound like you are casting a magic spell.
However, there are lots of fully studied science-backed connections between brain and body. And it’s worth knowing a bit of the basic anatomy on how they work.
To keep things basic, let’s come back to those two autonomic (or visceral) nervous systems. These are handled behind the scenes and not available for immediate control. Yes, there are methods such as meditation to access and switch them intentionally. But not in the same immediate way that you can think “squeeze my fist.” And lo and behold, it instantly squeezes. We’ll get to ways that you can “talk” to these systems later on in Part 2. And how massage for stress and PTSD can help. But for now treat them as automatic and out of your control.
Figure 1 shows the basics of what each of these nervous systems “do.”
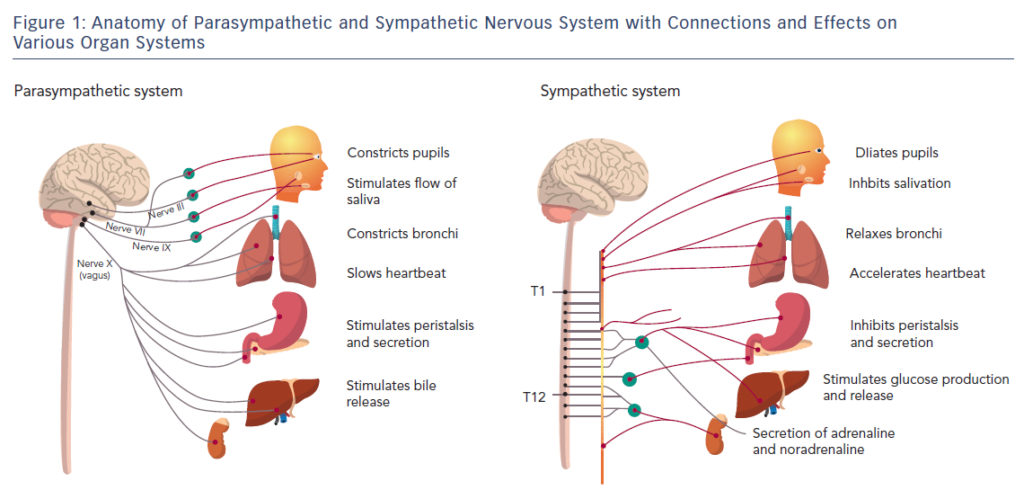
Parasympathetic on the left is for “rest & digest” – Sympathetic on the right is for “freeze, flight, fight”
Both of these systems connect your body to your central nervous system (or CNS). This is comprised of your brain and spinal cord. This allows for the body to quickly adjust to the demands you put on it. They act as “either/or” meaning both can’t be activated at the same time. This is hardwired and necessary for survival. For instance, it would be a very poor use of the body’s resources to try to digest food while also running away from a tiger. Neither function (digesting or running) would be performed at it’s best. And if you really had to stop to go to the bathroom…you’d get eaten.
Conversely, if you have managed to get to safety and finally eat a meal, it would be a poor use of resources to keep your heart rate up. And continue to pump you full of adrenaline. You wouldn’t be able to relax enough to fall asleep and fully restore your systems. Digestion happens best during the night when sleeping, so your digestion would also suffer. Those of you with chronic insomnia or IBS might want to check in with this. How can you create a safe “cave” experience at the end of your day to really restore?
Running on Instincts
Another thing to notice about the charts…your sympathetic nervous system connects directly to your spinal cord. And not to your brain. This allows it to react quickly and “on instinct.” Which is totally great for survival if you need a burst of physical power to survive an attack. You wouldn’t want to have to “think” through how to grab a tree branch if you were falling off a cliff. The extra split second it would take for your brain to respond might make all the difference to your survival. So evolution routed our danger response through our spinal cord instead to bypass the brain and speed up reaction time.
The problem is that our systems are still designed to interpret upset as signalling physical danger. When we are physically in danger, our instincts will generally give a higher survival rate than thinking things through. However, this mostly isn’t relevant or helpful in modern life. Most modern problems won’t be solved by hiding, running, or fighting.
So chronic stress can impede our higher brain functions to some degree resulting in more “thoughtless” behavior.
Improving Breathing: where massage for stress can really help
Look again at the list of things that both systems do when engaged. Most of these actions are totally out of your control. I dare you to make your pupils dilate or make your liver produce glucose on command. Go on, I’ll wait…..
However, there is one main function that you CAN control, actively and immediately. And that is how you breath.
Breathing is one of the few bodily functions that crosses over between your autonomic nervous system and your somatic nervous system. The somatic nervous system is the one attached to most of your muscles, skin, and joints. It’s for movement and interacting with your environment. You can hold your breath for a certain length of time. When you do this, you are using your somatic nervous system to exert control over your diaphragm. And over other breathing muscles to inhibit them from acting. Of course, since your autonomic nervous system is also attached, a fail-safe will kick in and take over. And make you breath again regardless of your desire to hold your breath.
You can’t directly control your heart, or the muscles in your organs. But you can control your diaphragm. Why might we be designed that way?
Think about when you watch a scary movie, and the killer is stalking someone who’s hiding. They are holding their breath in anticipation. Likely you are too even if you aren’t aware of it. This isn’t an accident even though it’s usually unconscious. You know the killer is listening and watching for you and would pick up on your breathing. So you hold it, by exerting somatic control over your diaphragm muscle.
There are actually two ways this happens. One is straight up holding and not breathing at all. For most of us, that won’t last more than a minute or so before our body forces us to breath.
The second is a much shallower form of breathing using your ancillary breathing muscles more and your diaphragm less. These ancillary breathing muscles include your scalenes, serratus muscles, intercostals, among others. This allows you to still take in oxygen, but much quieter and with much less movement in your ribcage.
This second way of “stress breathing” is a carry over from our primitive survival programs.
Stress breathing helps us hide from stalking predators. Who would otherwise pick up on the sound or ribcage movement of normal breathing. BTW, it also hides us from prey as we stalk them as well. So your body engages this stress breathing whenever you are focused on reaching a goal.
It triggers under just about any type of stress. Worried about what your boss will think of your report due Monday? Your body will trigger this type of stress breathing, even though it really does not do you any good. And actually will do you harm over time.
Massage for Stress and PTSD can help reset normal breathing and allow rest and relaxation again
I hesitate to use the words “normal breathing” as they imply there is one “correct” way to breath. As I like to say, “there is not one correct way to breath. But there are lots of incorrect ways.” What I mean is that “normal breathing” is not controlled and it’s not even. It’s flexible, and varies naturally without effort or thought with your activity levels. You have a brain stem that is designed to handle your breathing for you. It might be slow and shallow if you are sitting on the couch watching TV. Or fast and deep if you are exercising. Or anywhere in between. When it’s acting “normally” it fluidly changes to give you the right amount of oxygen with the least amount of effort.
We hear about all sorts of “correct” ways to breath:
- slow and deep,
- in through the nose out through the mouth,
- in through the nose out through the nose,
- equal length for inhale and exhale, etc.
All of these can controlled breathing patterns be “wrong” in the sense that they are control patterns.
In these “correct” ways to breath, you are trying to enforce a singular pattern of breath on all situations. And in doing so, using effort and control where none is needed. It actually requires force, ie muscular contraction, which costs calories and energy. And creates extra muscular tension that isn’t necessary.
Sure, exerting control over your breathing can give you a sense of…well, control. Which you might equate with safety. It can certainly help manage emotions, which can feel like you are managing stress. But we all need to stop equating “not freaking out” with “relaxing.”
Guess what actually happens when you try to control your breath?
Your brain interprets this is you either hiding from a predator or stalking prey. And engages your sympathetic nervous system, upping your body’s stress responses. Even though you feel less emotional, you are physiologically more stressed. And holding tension, engaging in hiding while being ready to run or fight at a moment’s notice.
Of course, if you are someone prone to wild emotional swings and out of control behavior, learning breath control techniques can absolutely help balance these out. Everything is relative.
However, if you tend towards even, sustained control and constant drive, you probably need to practice far less breath control.
I see many many NYC clients who literally can’t stop controlling their breath. No matter what they are feeling they’ve got it under constant and even control. To the point where it is an unconscious habit. This is absolutely one of my major red flags for chronic stress, ie running in sympathetic mode all the time. If you are wondering why in your 30’s you feel like “all of sudden I’m falling apart….” this is you.
You’ve been running the pedal to the metal for months to years (to decades). And now you are starting to get wear and tear injuries. Cortisol has been masking the underlying pains all this time. So you don’t notice that you need recovery until things truly blow out. Such as rotator cuff tears, plantar fasciitis, meniscus tears in your knee, stress fractures in your feet, etc.
And once the first injury happens, they start piling onto each other. Quickly.
Helping clients to let go of breath control is a first major step in healing. It allows you to switch on your parasympathetic nervous systems and get true rest. We can often get this to happen in your first session with direct work on the diaphragm and ribcage. As well as some directed awareness exercises on how you are holding and controlling the breath. For some of you it takes a few sessions. But once we can trigger this switch, your brain notices the difference. Once it gets a taste of rest and healing, it wants more. And starts to engage the switch more regularly.
FYI, giving up a bit of this type of control might bring on some emotions. Especially ones you’ve been working so hard to avoid. This is totally okay, and very good for your health. This often needs to happen first before your body can truly relax into parasympathetic mode.
So it’s not unusual for a client to have a short cry for no logical reason on the table.
Or bust out laughing. Or cursing for a bit and feeling anger. Sometimes it’s a mix of all three. As massage therapists, we are used to it. We always work to create a safe environment for you to have a mini breakdown. This will lead to a breakthrough of relaxation unlike anything you’ve likely experienced in a long time. Sometimes it doesn’t happen on the table but later.
Within several sessions you’ll gain the ability and tools to get to this restful state on your own. Which over time allows your body to heal itself more easily. It also makes the subsequent massage for stress and PTSD sessions far more effective. And this allows us to spend more time focusing on the specific issues. Including muscles, scar tissue, and holding patterns that cause localized injury and pain.
For PTSD clients, this work can help balance the threshold for triggering fight or flight to a more healthy level. Symptoms lessen and dissipate over time. And alongside working with a mental health professional, can speed up recovery immensely.
If you are dealing with symptoms from chronic stress and/or PTSD, we’d love to help with massage for stress and PTSD!
Massage for stress and PTSD alone isn’t going to solve all of your symptoms. But it can be an important part of your recovery. Alongside therapy with a mental health professional, massage can make a huge difference. Book a massage for chronic stress or PTSD in either our Financial District or Midtown West studios. We recommend working with either me (David) or a lead or senior therapist at first. We have more training and experience in this type of work. Do you have any questions about your specific case? Feel free to email us at hello@bodyworksdw.com or leave a comment in the comments section below.
In part 2, David will go into more depth on what sorts of symptoms and behaviors might indicate you have dealing with chronic stress and/or PTSD, and some self care practices that can help to manage it! Check in soon….